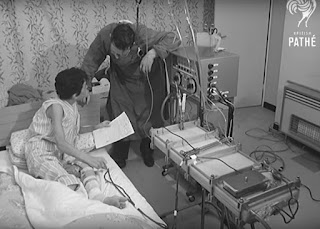
The first home haemodialysis, 1964
In the early 1960s dialysis was still a very new technology. It was high-tech, life-saving and dramatic. That you can run the the blood of conscious patients through a machine to replace a critical body function is still pretty amazing today. The idea of sending patients home to look after such a new, high-tech treatment themselves themselves must have seemed extraordinary. But dialysis was very expensive, and soon renal units were wrestling with how to stretch their resources to treat as many patients as possible.
The pressures led to changes on renal units. Nurses took on tasks that were originally the responsibility of doctors, technicians shared work on the team, even patients shared the work. Dialysis moved to become a nurse-led team treatment. Ann Eady recalls how the pressure of increasing numbers led to a transfer of the job of needling the fistula at Guy’s hospital. These radical changes in renal units probably had much further reaching consequences in medicine than we generally appreciate.
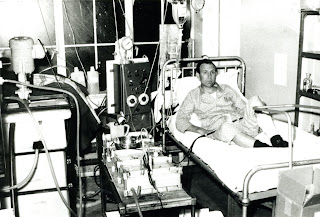

Ray Jones started treatment in 1963 via indwelling arterial and venous femoral catheters, one of the ‘Lucky 13’ at London’s Royal Free Hospital. When he died in 1991 after 29 years of treatment he was the longest surviving haemodialysis patient of his day. (Thanks to Joan Jones and Kidney Research UK).
Nancy Spaeth began treatment aged 18 in Seattle in 1966, switched to home dialysis in 1968 (pictured in 1969), and has experienced every modality of renal replacement therapy since. She is an active advocate for kidney patients today. (Courtesy of Nancy Spaeth)
However these changes were not enough. Staff salary costs still kept dialysis expensive, and units became physically full. Patients were mostly young, and had to be capable of working to be accepted for dialysis, but even then there was not capacity to treat those who needed it. For those lucky enough to be accepted, combining dialysis with work and family life were as difficult as they are now. However transplantation was a very high-risk gamble and if it failed you might not get back onto dialysis.
Haemodialysis carried out at home was introduced in three units thousands of miles apart in 1964, all responding to the same pressures. In Boston (Merrill) in July, Seattle (Scribner) in September, and in London (Shaldon) in October a patient received unattended overnight home dialysis for the first time. All used Scribner shunts. Some used machines made by patients families, and some of the early patients were healthcare professionals, but quickly the spread widened. In the same year, Boen reported visiting a patient at home in Seattle to carry out intermittent PD by repeated puncture using a rigid catheter. However it was to be two more decades before peritoneal dialysis could become established as a realistic medium to long term home option.
Some of the earliest UK home dialysis patients appear in the first episode of Tomorrow’s World 45 years ago (7th July 1965), available on the BBC website, but that was filmed at the Royal Free Hospital’s unit. A remarkable Pathe newsreel the same year shows Olga Heppell dialysing at home in Harlow. Her machine was in part manufactured by her husband.
MECHANICAL KIDNEY SAVES WIFE’S LIFE – from British Pathe newsreel, or YouTube link
In 1965 Stanley Shaldon reported that giving the work to patients in the unit, primarily as a cost-saving measure, led to an increase in quality of care and in patients’ independence. By 1968 he was writing about the additional benefits in independence and quality of life from home haemodialysis. Has this changed? Probably not.
Now home haemodialysis is on the rise again. The blogosphere is filled with enthusiastic accounts from patients doing daily dialysis at home, reporting much better health and quality of life. Machines are moving toward supporting home haemodialysis better. Getting the numbers really high again is made challenging by the different profile of patients today: older, with more comorbidities and greater dependencies. But it was always the best long term treatment if you couldn’t get a safe transplant, and it probably still is.
Further information
Cameron JS 2002. A history of the treatment of renal failure by dialysis. Oxford University Press, Oxford
Wellcome Witness to the History of Medicine 2009. History of dialysis in the UK.
Spaeth N 2007. The nurse, mother of two and four transplants – Nancy Spaeth tells her story. Nephrol Dial Transplant 22:64-7
First episode of the BBC TV programme Tomorrow’s World in 1965
This post will be published in the Journal of Renal Nursing in July 2010.